Home › Gut health and digestion
Gut health and digestion
The gut microbiome changes significantly at menopause — and those changes affect everything from digestion and bloating to mood, weight, inflammation, and even how the body processes estrogen. One of the most underrecognised areas of menopausal health.

Rose
"The bloating that arrived in my 40s without explanation was one of the first signs something was changing hormonally — long before my periods became irregular. Nobody mentioned the gut-hormone connection. Understanding it changed how I eat, what I supplement, and how I think about my digestive symptoms."
Key takeaways
✓Estrogen receptors line the entire gut — its decline slows motility, reduces microbiome diversity, and increases gut permeability simultaneously
✓The estrobolome (gut bacteria that process estrogen) is disrupted at menopause — supporting it with fermented food and fibre is one of the most direct hormonal dietary interventions
✓Fermented foods have the strongest evidence — rotate between kimchi, kefir, sauerkraut, and tempeh for bacterial diversity
✓Bloating at menopause is hormonal, not just dietary — slower motility and heightened visceral sensitivity mean you feel distension at much lower thresholds than before
✓Start with food before supplements — fibre and fermented foods outperform most probiotic supplements in current evidence
The gut-hormone connection
How menopause changes the gut
Estrogen receptors are distributed throughout the gastrointestinal tract — in the gut lining, in smooth muscle, and in the enteric nervous system. Estrogen influences gut motility (how quickly food moves through), gut barrier integrity, pain sensitivity, and the composition of the gut microbiome. When estrogen declines, all of these change simultaneously.
Gut motility slows
Progesterone decline removes its muscle-relaxing effect — constipation becomes more common
Microbiome diversity falls
Estrobolome — the gut bacteria that metabolise estrogen — changes significantly at menopause
Gut permeability increases
The gut lining becomes more permeable, increasing inflammation and food sensitivity
Visceral sensitivity rises
The gut becomes more sensitive to normal amounts of gas and distension — causing pain and discomfort at lower thresholds
The estrobolome — the gut bacteria that process estrogen
A specific group of gut bacteria called the estrobolome produces an enzyme (beta-glucuronidase) that influences how estrogen is metabolised and reabsorbed in the gut. An unhealthy estrobolome leads to inefficient estrogen clearance and erratic estrogen recirculation. This contributes to estrogen dominance in perimenopause, worsens symptoms, and affects long-term hormonal balance. Supporting the estrobolome with fermented foods, fibre, and probiotics is one of the most direct dietary interventions for menopausal hormonal health.
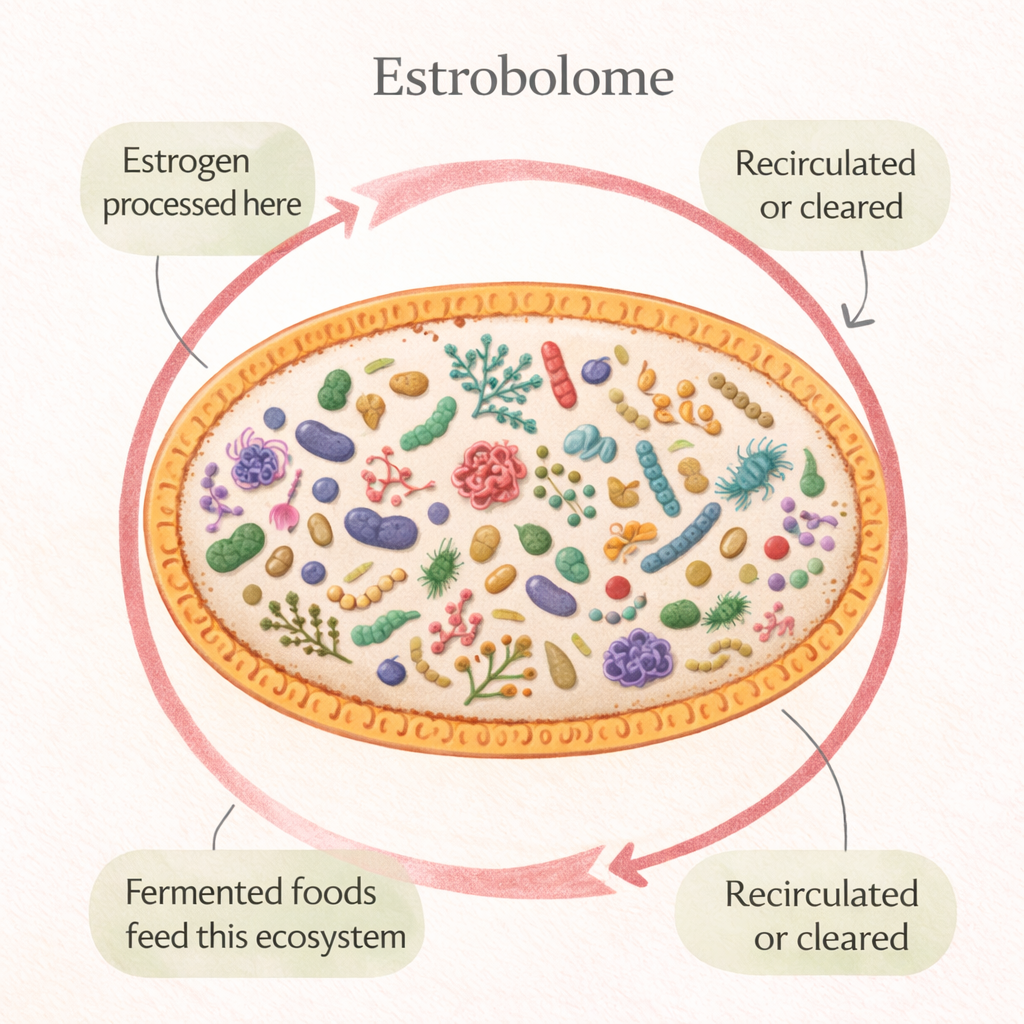
Fermented foods — the most direct intervention
Strong evidence
Kimchi, sauerkraut, kefir, tempeh, and natural yogurt deliver live bacteria directly to the gut. A Stanford study showed that a high-fermented-food diet increased microbiome diversity and reduced inflammatory markers more effectively than a high-fibre diet alone. For menopausal women, variety matters — rotate between different fermented foods to diversify bacterial strains.
Practical
Start with 1-2 tablespoons of sauerkraut or kimchi daily and build up gradually. Introduce slowly — too much too fast causes bloating.
Dietary fibre — feeding the right bacteria
Strong evidence
Prebiotic fibre — from onions, garlic, leeks, asparagus, oats, and legumes — feeds the beneficial bacteria in the gut. Fibre intake in Western women is typically 10-15g daily against a recommended 25-30g. Increasing fibre directly supports estrobolome health and reduces constipation.
Practical
Add one extra serving of legumes, extra portion of vegetables, or oats daily. Increase gradually over 2-3 weeks to allow the microbiome to adjust.
Reducing gut inflammation
Mixed evidence
Ultra-processed foods, refined sugar, and industrial seed oils promote gut inflammation and disrupt the gut lining. Eliminating these is the single most impactful dietary change for gut health — not because of the nutrients you add but because of the damage you stop causing.
Practical
The practical test: if it has more than 5 ingredients or contains ingredients you would not find in a kitchen, it is likely ultra-processed.
Targeted probiotic supplementation
Mixed evidence
Lactobacillus and Bifidobacterium strains have the most evidence for menopausal gut health. Specific strains of interest: Lactobacillus acidophilus and Lactobacillus rhamnosus for gut lining integrity; Bifidobacterium longum for mood via the gut-brain axis. The evidence for specific strains is growing but not yet definitive.
Practical
Refrigerated multi-strain probiotics with at least 10 billion CFU. Consistency over weeks matters more than dose. Food-based sources (kefir, yogurt) have better evidence than most supplements.
L-glutamine for gut lining repair
Mixed evidence
L-glutamine is the primary fuel for gut lining cells and supports the tight junctions that maintain gut barrier integrity. Used by integrative practitioners for increased gut permeability (leaky gut). Evidence is mostly mechanistic with limited large trials.
Practical
5-10g daily mixed in cool water on an empty stomach. Start at 5g and increase slowly.
Managing bloating specifically
Why bloating gets worse at menopause
Menopausal bloating is driven by three simultaneous changes: slower gut motility (food sits longer, fermenting longer), increased visceral sensitivity (the gut feels distension more acutely), and microbiome changes that alter fermentation patterns. The result is bloating that feels out of proportion to what was eaten. This is not imagined and it is not solely about food choices — it is hormonal.
Practical approaches to bloating
• Eat slowly and chew thoroughly — the most evidence-backed and most ignored advice
• Do not eat large meals late in the evening — gut motility slows overnight
• Identify personal trigger foods — common triggers include cruciferous vegetables at high volume, legumes, lactose, and carbonated drinks
• Move after meals — a 10-15 minute walk significantly accelerates gut motility
• Peppermint tea or enteric-coated peppermint oil capsules — good evidence for reducing bloating and gut spasm
• Consider a short low-FODMAP trial if bloating is severe — under dietitian guidance
Rose on this
"Gut health in menopause is one of those areas where the lifestyle interventions genuinely work — more fermented food, more fibre, less ultra-processed food. The research is catching up to what women have observed for years. Start with food before supplements. The gut responds faster than most people expect."
From Rose
"The gut-brain connection is real in a way I did not appreciate until I was in it. When my gut is unhappy my mood is worse, my brain fog is worse, and my sleep is worse. When my gut is well my whole system settles. The microbiome is not a wellness trend — it is a central part of how the menopausal body works."
What we do not know yet
?Which probiotic strains are optimal long-term for the menopausal estrobolome — the evidence is growing but not yet definitive for specific strain combinations
?Whether estrobolome testing is clinically reliable enough to guide individual supplementation — most commercial tests are not yet validated for this use
?The optimal dose and duration of L-glutamine for gut lining repair in menopausal women specifically — current evidence is mostly mechanistic
?How much of the gut microbiome change at menopause is driven by hormones versus ageing — the two are difficult to separate in study design
Whole grains — fibre and the gut ›
Bloating and digestive changes ›
Gut-supportive recipes ›
Dietary patterns for menopause ›
Written by

Rose
Navigating perimenopause · Researcher · Founded rosemyfriend.com
Research basis
PubMed · Cochrane reviews · NICE guidelines · British Menopause Society · The Menopause Society
Read methodology →
Last updated
March 2026
Rose provides evidence-graded educational information — not medical advice. Always discuss health decisions with a qualified healthcare provider. Full disclaimer · About Rose